The science behind Integral Biotics®
WHAT ARE PSYCHOBIOTICS?
Psychobiotics are live microorganisms that produce beneficial effects on mental health when consumed in adequate amounts. They work by altering chemistry of the brain and increasing levels of certain neurotransmitters that control mood and behaviour. These special probiotics change how we react to stress and regulate our moods.
Psychobiotics are beneficial because they can help to reduce stress and anxiety, increase positive emotions and improve cognitive functioning. Research has also shown that they may be able to treat certain mental illnesses such as depression or anxiety disorders.
The properties of psychobiotics exist thanks to their interactions within the gut-brain axis.
GUT-BRAIN AXIS
The gut-brain axis is a bidirectional communication system that involves the brain and the gastrointestinal tract. There are nerves that communicate between these two organs, letting them know what’s happening with one another. It’s all happening thanks to the longest nerve of the autonomic nervous system- the vagus nerve that delivers the information between the central nervous system and the gut.
The gut-brain axis is a key component of human physiology. It’s a complex network of tissues and organs working together to develop and maintain optimal health.The gut influences and is influenced by neural, immune, endocrine and metabolic factors that pass along the systemic circulation, thereby providing an important link between physical and mental health. The gut plays a crucial role in our well-being, with many vital functions such as food absorption, producing vitamins and helping to fight infection. It is also home to trillions of microorganisms – collectively referred to as the microbiome – that help us digest food, maintain our immune system and fight off infections. As many as 100 trillion bacteria live in the gastrointestinal tract, which represents almost half of the body’s immune system.
It has been demonstrated that probiotics have broader therapeutic applications than previously considered. There are hundreds of studies showing how gut health affects our moods, emotions, behaviour and cognition. It works by altering brain chemistry and increasing levels of certain neurotransmitters in the brain that control mood and behaviour. Live microorganisms that can produce beneficial effects on mental health are called psychobiotics.
NERVOUS SYSTEM
Microbiome exerts its action through the enteric nervous system (ENS). The ENS is the largest and most complex division of the peripheral and autonomic nervous systems. It contains many different types of neurons comparable in number to that of the spinal cord and an array of neurotransmitters and neuromodulators similar to those found in the central nervous system (CNS). Both the vagus nerve and modulation of systemic tryptophan levels are strongly implicated in the influence that the gut microbiota has on the brain.
Bacteria have the capacity to generate many neurotransmitters and neuromodulators. It has been determined that selective psychobiotic bacteria strains have an ability to produce serotonin, dopamine, acetylcholine or GABA, all of which play an important role in motivation, mood and cognitive functioning.
IMMUNE SYSTEM
Microbiota plays an important role in immune system regulation via anti-inflammatory mechanisms that can counteract immune-mediated CNS disease symptoms. The gut microbiota and psychobiotics can alter the levels of circulating cytokines, and this can have a significant effect on brain function.
Microbiota and psychobiotics can have direct effects on the immune system. The immune system also exerts a bidirectional communication with the CNS making it a prime target for transducing the effects of bacteria on the CNS. In addition, indirect effects of the gut microbiota and probiotics on the innate immune system can result in alterations in the circulating levels of pro-inflammatory and anti-inflammatory cytokines that directly affect brain function.

NEUROENDOCRINE SYSTEM
In the endocrinal pathway, the gut microbiome plays a major role in the development and regulation of the hypothalamus-pituitary-adrenal (HPA) axis that is critical to stress response. Endocrine cells secrete neurotransmitters in response to luminal stimuli, acting as transducers for the gut-endocrine-CNS route. The HPA axis regulates cortisol secretion that can affect immune cells (including cytokine secretion) both locally in the gut and systemically. Cortisol can also alter gut permeability and barrier function, and change gut microbiota composition.
Many studies highlight a role of the microbiota in modulating the stress response and in modulating stress-related behaviours that are relevant to psychiatric disorders such as anxiety and depression.
METABOLIC PATHWAY
Gut bacteria modulate various host metabolic reactions, resulting in the production of metabolites such as secondary bile acids, choline and short-chain fatty acids that are essential for host health. Indeed, complex carbohydrates such as dietary fibre can be digested and subsequently fermented in the colon by gut microorganisms into short-chain fatty acids such as n-butyrate, acetate and propionate, which are known to have neuroactive properties and can modulate brain and behaviour.
WHAT ARE PSYCHOBIOTICS?
Psychobiotics are live microorganisms that produce beneficial effects on mental health when consumed in adequate amounts. They work by altering chemistry of the brain and increasing levels of certain neurotransmitters that control mood and behaviour. These special probiotics change how we react to stress and regulate our moods.
Psychobiotics are beneficial because they can help to reduce stress and anxiety, increase positive emotions and improve cognitive functioning. Research has also shown that they may be able to treat certain mental illnesses such as depression or anxiety disorders.
The properties of psychobiotics exist thanks to their interactions within the gut-brain axis.

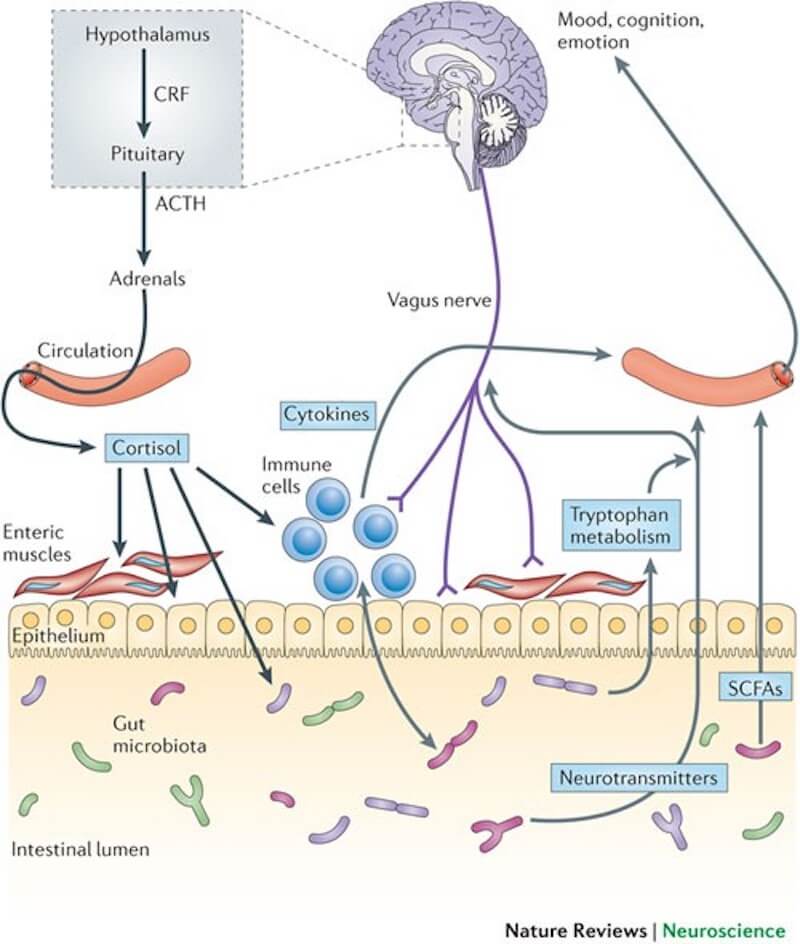
GUT-BRAIN AXIS
The gut-brain axis is a bidirectional communication system that involves the brain and the gastrointestinal tract. There are nerves that communicate between these two organs, letting them know what’s happening with one another. It’s all happening thanks to the longest nerve of the autonomic nervous system- the vagus nerve that delivers the information between the central nervous system and the gut.
The gut-brain axis is a key component of human physiology. It’s a complex network of tissues and organs working together to develop and maintain optimal health.The gut influences and is influenced by neural, immune, endocrine and metabolic factors that pass along the systemic circulation, thereby providing an important link between physical and mental health. The gut plays a crucial role in our well-being, with many vital functions such as food absorption, producing vitamins and helping to fight infection. It is also home to trillions of microorganisms – collectively referred to as the microbiome – that help us digest food, maintain our immune system and fight off infections. As many as 100 trillion bacteria live in the gastrointestinal tract, which represents almost half of the body’s immune system.

It has been demonstrated that probiotics have broader therapeutic applications than previously considered. There are hundreds of studies showing how gut health affects our moods, emotions, behaviour and cognition. It works by altering brain chemistry and increasing levels of certain neurotransmitters in the brain that control mood and behaviour. Live microorganisms that can produce beneficial effects on mental health are called psychobiotics.

NERVOUS SYSTEM
Microbiome exerts its action through the enteric nervous system (ENS). The ENS is the largest and most complex division of the peripheral and autonomic nervous systems. It contains many different types of neurons comparable in number to that of the spinal cord and an array of neurotransmitters and neuromodulators similar to those found in the central nervous system (CNS). Both the vagus nerve and modulation of systemic tryptophan levels are strongly implicated in the influence that the gut microbiota has on the brain.
Bacteria have the capacity to generate many neurotransmitters and neuromodulators. It has been determined that selective psychobiotic bacteria strains have an ability to produce serotonin, dopamine, acetylcholine or GABA, all of which play an important role in motivation, mood and cognitive functioning.
IMMUNE SYSTEM
Microbiota plays an important role in immune system regulation via anti-inflammatory mechanisms that can counteract immune-mediated CNS disease symptoms. The gut microbiota and psychobiotics can alter the levels of circulating cytokines, and this can have a significant effect on brain function.
Microbiota and psychobiotics can have direct effects on the immune system. The immune system also exerts a bidirectional communication with the CNS making it a prime target for transducing the effects of bacteria on the CNS. In addition, indirect effects of the gut microbiota and probiotics on the innate immune system can result in alterations in the circulating levels of pro-inflammatory and anti-inflammatory cytokines that directly affect brain function.

NEUROENDOCRINE SYSTEM
In the endocrinal pathway, the gut microbiome plays a major role in the development and regulation of the hypothalamus-pituitary-adrenal (HPA) axis that is critical to stress response. Endocrine cells secrete neurotransmitters in response to luminal stimuli, acting as transducers for the gut-endocrine-CNS route. The HPA axis regulates cortisol secretion that can affect immune cells (including cytokine secretion) both locally in the gut and systemically. Cortisol can also alter gut permeability and barrier function, and change gut microbiota composition.
Many studies highlight a role of the microbiota in modulating the stress response and in modulating stress-related behaviours that are relevant to psychiatric disorders such as anxiety and depression.

METABOLIC PATHWAY
Gut bacteria modulate various host metabolic reactions, resulting in the production of metabolites such as secondary bile acids, choline and short-chain fatty acids that are essential for host health. Indeed, complex carbohydrates such as dietary fibre can be digested and subsequently fermented in the colon by gut microorganisms into short-chain fatty acids such as n-butyrate, acetate and propionate, which are known to have neuroactive properties and can modulate brain and behaviour.
As shown, psychobiotics work in a very holistic way affecting many different parts of the body and addressing both physical and mental health.
GUT-BRAIN AXIS
The gut-brain axis is a bidirectional communication system that involves the brain and the gastrointestinal tract. There are nerves that communicate between these two organs, letting them know what’s happening with one another. It’s all happening thanks to the longest nerve of the autonomic nervous system- the vagus nerve that delivers the information between the central nervous system and the gut.
The gut-brain axis is a key component of human physiology. It’s a complex network of tissues and organs working together to develop and maintain optimal health.The gut influences and is influenced by neural, immune, endocrine and metabolic factors that pass along the systemic circulation, thereby providing an important link between physical and mental health. The gut plays a crucial role in our well-being, with many vital functions such as food absorption, producing vitamins and helping to fight infection. It is also home to trillions of microorganisms – collectively referred to as the microbiome – that help us digest food, maintain our immune system and fight off infections. As many as 100 trillion bacteria live in the gastrointestinal tract, which represents almost half of the body’s immune system.
It has been demonstrated that probiotics have broader therapeutic applications than previously considered. There are hundreds of studies showing how gut health affects our moods, emotions, behaviour and cognition. It works by altering brain chemistry and increasing levels of certain neurotransmitters in the brain that control mood and behaviour. Live microorganisms that can produce beneficial effects on mental health are called psychobiotics.

(Cryan, Dinan, 2012)
NERVOUS SYSTEM
Microbiome exerts its action through the enteric nervous system (ENS). The ENS is the largest and most complex division of the peripheral and autonomic nervous systems. It contains many different types of neurons comparable in number to that of the spinal cord and an array of neurotransmitters and neuromodulators similar to those found in the central nervous system (CNS). Both the vagus nerve and modulation of systemic tryptophan levels are strongly implicated in the influence that the gut microbiota has on the brain.
Bacteria have the capacity to generate many neurotransmitters and neuromodulators. It has been determined that selective psychobiotic bacteria strains have an ability to produce serotonin, dopamine, acetylcholine or GABA, all of which play an important role in motivation, mood and cognitive functioning.

NEUROENDOCRINE SYSTEM
In the endocrinal pathway, the gut microbiome plays a major role in the development and regulation of the hypothalamus-pituitary-adrenal (HPA) axis that is critical to stress response. Endocrine cells secrete neurotransmitters in response to luminal stimuli, acting as transducers for the gut-endocrine-CNS route. The HPA axis regulates cortisol secretion that can affect immune cells (including cytokine secretion) both locally in the gut and systemically. Cortisol can also alter gut permeability and barrier function, and change gut microbiota composition.
Many studies highlight a role of the microbiota in modulating the stress response and in modulating stress-related behaviours that are relevant to psychiatric disorders such as anxiety and depression.

IMMUNE SYSTEM
Microbiota plays an important role in immune system regulation via anti-inflammatory mechanisms that can counteract immune-mediated CNS disease symptoms. The gut microbiota and psychobiotics can alter the levels of circulating cytokines, and this can have a significant effect on brain function.
Microbiota and psychobiotics can have direct effects on the immune system. The immune system also exerts a bidirectional communication with the CNS making it a prime target for transducing the effects of bacteria on the CNS. In addition, indirect effects of the gut microbiota and probiotics on the innate immune system can result in alterations in the circulating levels of pro-inflammatory and anti-inflammatory cytokines that directly affect brain function.

METABOLIC PATHWAY
Gut bacteria modulate various host metabolic reactions, resulting in the production of metabolites such as secondary bile acids, choline and short-chain fatty acids that are essential for host health. Indeed, complex carbohydrates such as dietary fibre can be digested and subsequently fermented in the colon by gut microorganisms into short-chain fatty acids such as n-butyrate, acetate and propionate, which are known to have neuroactive properties and can modulate brain and behaviour.

As shown, psychobiotics work in a very holistic way affecting many different parts of the body and addressing both physical and mental health.
